How Gout Progresses and Who Is at Risk
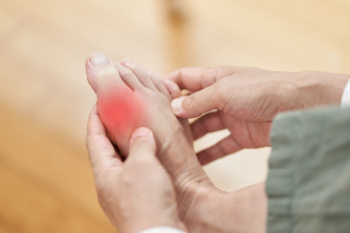
Gout, a type of arthritis characterized by sudden and severe pain attacks, can progress through four distinct stages, each posing unique challenges and implications for affected individuals. Initially, the asymptomatic hyperuricemia stage occurs, where elevated uric acid levels accumulate in the blood without any noticeable symptoms. This stage can persist for years before progressing to acute gouty arthritis, marked by sudden and intense joint pain, typically in the big toe. If left untreated, recurrent gout attacks may ensue, leading to the chronic gout stage characterized by frequent flare-ups and potential joint damage. In severe cases, tophaceous gout may develop, characterized by the formation of urate crystals in the joints and surrounding tissues, resulting in visible lumps. While anyone can develop gout, certain factors such as genetics, obesity, dietary habits rich in purines, alcohol consumption, and certain medications increase the risk. If you have developed gout, it is strongly suggested that you are under the care of a podiatrist who can determine which stage you are in, and offer effective relief options.
Gout is a painful condition that can be treated. If you are seeking treatment, contact Dr. Barbara Davis from Gilbert Podiatry. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
- Intense Joint Pain - Usually around the large joint of your big toe, and it most severe within the first four to twelve hours
- Lingering Discomfort - Joint discomfort may last from a few days to a few weeks
- Inflammation and Redness -Affected joints may become swollen, tender, warm and red
- Limited Range of Motion - May experience a decrease in joint mobility
Risk Factors
- Genetics - If family members have gout, you’re more likely to have it
- Medications - Diuretic medications can raise uric acid levels
- Gender/Age - Gout is more common in men until the age of 60. It is believed that estrogen protects women until that point
- Diet - Eating red meat and shellfish increases your risk
- Alcohol - Having more than two alcoholic drinks per day increases your risk
- Obesity - Obese people are at a higher risk for gout
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact our office located in Gilbert, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Treatment Options for Drop Foot

Foot drop is a condition marked by having difficulty lifting or moving the foot and toes. The foot fails to lift properly, causing a gait that looks like marching. Foot drop typically stems from nerve injuries as the result of sports injuries, spinal issues like slipped discs, or neuropathies associated with conditions such as diabetes. Other causes of drop foot include inherited conditions like Charcot-Marie-Tooth disease or neurological disorders, such as stroke or multiple sclerosis. Treatment strategies for foot drop are multifaceted, depending on the underlying cause and severity of symptoms. Certain exercises can play an important role in strengthening and stretching muscles to improve function. In addition, braces, splints, or custom orthotics may offer external support and aid in maintaining proper foot positioning. In cases of permanent impairment, surgical joint fusion or nerve repair may be necessary. Electrical nerve stimulation devices also can offer promising therapeutic options, particularly for individuals affected by stroke or multiple sclerosis. If you have symptoms of foot drop, it is suggested that you schedule an appointment with a podiatrist for an exam and diagnosis, followed by the appropriate treatment options.
If you have any concerns about your feet, contact Dr. Barbara Davis from Gilbert Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Biomechanics in Podiatry
Podiatric biomechanics is a particular sector of specialty podiatry with licensed practitioners who are trained to diagnose and treat conditions affecting the foot, ankle and lower leg. Biomechanics deals with the forces that act against the body, causing an interference with the biological structures. It focuses on the movement of the ankle, the foot and the forces that interact with them.
A History of Biomechanics
- Biomechanics dates back to the BC era in Egypt where evidence of professional foot care has been recorded.
- In 1974, biomechanics gained a higher profile from the studies of Merton Root, who claimed that by changing or controlling the forces between the ankle and the foot, corrections or conditions could be implemented to gain strength and coordination in the area.
Modern technological improvements are based on past theories and therapeutic processes that provide a better understanding of podiatric concepts for biomechanics. Computers can provide accurate information about the forces and patterns of the feet and lower legs.
Understanding biomechanics of the feet can help improve and eliminate pain, stopping further stress to the foot.
If you have any questions please feel free to contact our office located in Gilbert, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Trim Properly to Avoid Ingrown Toenails
 Improper toenail trimming is a common culprit behind ingrown toenails, a painful condition that occurs when the nail grows into the surrounding skin. The risk of ingrown toenails increases when toenails are trimmed improperly. This includes when toenails are cut too short, rounded at the corners, or not trimmed straight across. To trim toenails correctly and reduce the likelihood of ingrowth, you should follow a few simple steps. Firstly, soften the nails by soaking the feet in warm water for a few minutes. Using sanitized nail clippers, cut the nails straight across, avoiding curved edges. Ensure that the nails remain slightly longer than the skin at the nail's edge. Digging the clippers into the corners of the nails, or trying to create a rounded shape, will increase your chances of developing ingrown toenails. Adopting these toenail-trimming practices will help you maintain healthy, pain-free feet. If you suspect ingrowth, it is suggested you seek an appointment with a podiatrist, who can help you treat ingrown toenails and provide more prevention tips.
Improper toenail trimming is a common culprit behind ingrown toenails, a painful condition that occurs when the nail grows into the surrounding skin. The risk of ingrown toenails increases when toenails are trimmed improperly. This includes when toenails are cut too short, rounded at the corners, or not trimmed straight across. To trim toenails correctly and reduce the likelihood of ingrowth, you should follow a few simple steps. Firstly, soften the nails by soaking the feet in warm water for a few minutes. Using sanitized nail clippers, cut the nails straight across, avoiding curved edges. Ensure that the nails remain slightly longer than the skin at the nail's edge. Digging the clippers into the corners of the nails, or trying to create a rounded shape, will increase your chances of developing ingrown toenails. Adopting these toenail-trimming practices will help you maintain healthy, pain-free feet. If you suspect ingrowth, it is suggested you seek an appointment with a podiatrist, who can help you treat ingrown toenails and provide more prevention tips.
Ingrown toenails may initially present themselves as a minor discomfort, but they may progress into an infection in the skin without proper treatment. For more information about ingrown toenails, contact Dr. Barbara Davis of Gilbert Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails are caused when the corner or side of a toenail grows into the soft flesh surrounding it. They often result in redness, swelling, pain, and in some cases, infection. This condition typically affects the big toe and may recur if it is not treated properly.
Causes
- Improper toenail trimming
- Genetics
- Improper shoe fitting
- Injury from pedicures or nail picking
- Abnormal gait
- Poor hygiene
You are more likely to develop an ingrown toenail if you are obese, have diabetes, arthritis, or have any fungal infection in your nails. Additionally, people who have foot or toe deformities are at a higher risk of developing an ingrown toenail.
Symptoms
Some symptoms of ingrown toenails are redness, swelling, and pain. In rare cases, there may be a yellowish drainage coming from the nail.
Treatment
Ignoring an ingrown toenail can have serious complications. Infections of the nail border can progress to a deeper soft-tissue infection, which can then turn into a bone infection. You should always speak with your podiatrist if you suspect you have an ingrown toenail, especially if you have diabetes or poor circulation.
If you have any questions, please feel free to contact our office located in Gilbert, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Types of Arthritis Causing Ankle Pain
 There are many kinds of arthritis, and one of them could be a cause of your ankle pain. Osteoarthritis, the most common type, occurs when wear and tear on the cartilage that cushions the ends of the bones causes the bones to rub against each other. People with osteoarthritis in their ankle may experience painful joints between the shin and ankle. Rheumatoid arthritis, an autoimmune condition, often causes joint pain in both ankles. Gout is another type of arthritis that can cause ankle pain because of a buildup of uric acid in the body. Gout patients often feel pain in the big toe as one of their first symptoms. Sudden intense pain that lasts for several hours and affects any of the joints, including ankles, can indicate a gout attack. These are not the only forms of arthritis that can lead to ankle pain. Understanding the specific type of arthritis affecting the ankle is important for developing an effective treatment plan. If you are experiencing persistent ankle pain, it is suggested you consult a podiatrist who can help identify the underlying cause of your pain, diagnose types of arthritis, and explore appropriate treatment plans.
There are many kinds of arthritis, and one of them could be a cause of your ankle pain. Osteoarthritis, the most common type, occurs when wear and tear on the cartilage that cushions the ends of the bones causes the bones to rub against each other. People with osteoarthritis in their ankle may experience painful joints between the shin and ankle. Rheumatoid arthritis, an autoimmune condition, often causes joint pain in both ankles. Gout is another type of arthritis that can cause ankle pain because of a buildup of uric acid in the body. Gout patients often feel pain in the big toe as one of their first symptoms. Sudden intense pain that lasts for several hours and affects any of the joints, including ankles, can indicate a gout attack. These are not the only forms of arthritis that can lead to ankle pain. Understanding the specific type of arthritis affecting the ankle is important for developing an effective treatment plan. If you are experiencing persistent ankle pain, it is suggested you consult a podiatrist who can help identify the underlying cause of your pain, diagnose types of arthritis, and explore appropriate treatment plans.
Ankle pain can be caused by a number of problems and may be potentially serious. If you have ankle pain, consult with Dr. Barbara Davis from Gilbert Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Ankle pain is any condition that causes pain in the ankle. Due to the fact that the ankle consists of tendons, muscles, bones, and ligaments, ankle pain can come from a number of different conditions.
Causes
The most common causes of ankle pain include:
- Types of arthritis (rheumatoid, osteoarthritis, and gout)
- Ankle sprains
- Broken ankles
- Achilles tendinitis
- Achilles tendon rupture
- Stress fractures
- Bursitis
- Tarsal tunnel syndrome
- Plantar fasciitis
Symptoms
Symptoms of ankle injury vary based upon the condition. Pain may include general pain and discomfort, swelling, aching, redness, bruising, burning or stabbing sensations, and/or loss of sensation.
Diagnosis
Due to the wide variety of potential causes of ankle pain, podiatrists will utilize a number of different methods to properly diagnose ankle pain. This can include asking for personal and family medical histories and of any recent injuries. Further diagnosis may include sensation tests, a physical examination, and potentially x-rays or other imaging tests.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are rest, ice packs, keeping pressure off the foot, orthotics and braces, medication for inflammation and pain, and surgery.
If you have any questions, please feel free to contact our office located in Gilbert, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Definition and Symptoms of an Achilles Tendon Injury

The Achilles tendon, a strong band of tissue connecting the calf muscles to the heel bone, plays a pivotal role in facilitating movement. An Achilles tendon injury refers to the damage or inflammation that occurs in this critical structure, impacting the ability to walk, run, or perform various physical activities. Typically, injuries to the Achilles tendon manifest as pain, swelling, and stiffness, often concentrated near the back of the heel. Individuals may experience difficulty pointing their toes or pushing off the ground. The discomfort can range from mild to severe, and in some cases, a noticeable thickening of the tendon may be observed. Achilles tendon injuries are frequently associated with overuse, sudden increases in physical activity, or inadequate warm-up routines. If you have endured an Achilles tendon injury, it is suggested that you confer with a podiatrist who can guide you toward the correct treatment method.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact Dr. Barbara Davis of Gilbert Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our office located in Gilbert, PA . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Podiatry and Rheumatoid Arthritis

Podiatry is a specialized medical field dedicated to evaluating, diagnosing, and addressing issues related to the feet and ankles. Practitioners who hold specialized or extended roles in podiatry are well-equipped to provide expert assessment, guidance, and treatment for individuals dealing with all types of foot and ankle problems, including rheumatoid arthritis, or RA. Among patients affected by RA, podiatric care is a highly sought-after service. Podiatrists possess the knowledge and skills required to understand the unique challenges posed by rheumatic diseases on the feet and ankles. These doctors play a critical role in managing the foot-related aspects of RA, offering patients comprehensive care to alleviate pain, improve mobility, and enhance their overall quality of life. If you suffer from rheumatoid arthritis that is impacting your feet and ankles, it is suggested that you schedule an appointment with a podiatrist for treatment.
Because RA affects more than just your joints, including the joints in your feet and ankles, it is important to seek early diagnosis from your podiatrist if you feel like the pain in your feet might be caused by RA. For more information, contact Dr. Barbara Davis of Gilbert Podiatry. Our doctor will assist you with all of your podiatric concerns.
What Is Rheumatoid Arthritis?
Rheumatoid Arthritis (RA) is an autoimmune disorder in which the body’s own immune system attacks the membranes surrounding the joints. Inflammation of the lining and eventually the destruction of the joint’s cartilage and bone occur, causing severe pain and immobility.
Rheumatoid Arthritis of the Feet
Although RA usually attacks multiple bones and joints throughout the entire body, almost 90 percent of cases result in pain in the foot or ankle area.
Symptoms
- Swelling and pain in the feet
- Stiffness in the feet
- Pain on the ball or sole of feet
- Joint shift and deformation
Diagnosis
Quick diagnosis of RA in the feet is important so that the podiatrist can treat the area effectively. Your doctor will ask you about your medical history, occupation, and lifestyle to determine the origin of the condition. Rheumatoid Factor tests help to determine if someone is affected by the disease.
If you have any questions please feel free to contact our office located in Gilbert, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Causes and Symptoms of Turf Toe

Turf toe is a common injury that often strikes athletes such as football players, dancers and gymnasts, with a sudden and traumatic onset. Most recall the precise moment it occurred. Turf toe results in pain around the ball of the foot, particularly on the bottom of the metatarsophalangeal, or MTP, joint, just below the big toe. Those experiencing turf toe may note pain with or without movement. It can be felt when the toe is flexed to the extreme or during the toe-off phase of walking. Swelling of the MTP joint may accompany the pain, along with a decrease in strength and range of motion. The affected joint also may become warm and tender to the touch. Turf toe can cause a noticeable lump or gap, and what is described as a crunchy feeling due to inflammation. Difficulty walking and maintaining balance can result from the pain and loss of function in the affected joints and surrounding tissues. If you suspect a turf toe injury, it is suggested that you schedule an appointment with a podiatrist for an exam and accurate diagnosis. A tailored treatment plan can help you get back in the game.
Toe pain can disrupt your daily activities. If you have any concerns, contact Dr. Barbara Davis of Gilbert Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Causes Toe Pain?
Most severe toe pain is caused due to a sports injury, trauma from dropping something heavy on the toe, or bumping into something rigid. Other problems can develop over time for various reasons.
Toe pain can be caused by one or more ailments. The most common include:
- Trauma
- Sports injury
- Wearing shoes that are too tight
- Arthritis
- Gout
- Corns and calluses
- Hammertoe
- Bunions
- Blisters
- Ingrown toenails
- Sprains
- Fractures (broken bones)
- Dislocations
When to See a Podiatrist
- Severe pain
- Persistent pain that lasts more than a week
- Signs of infection
- Continued swelling
- Pain that prevents walking
Diagnosis
In many cases the cause of toe pain is obvious, but in others, a podiatrist may want to use more advanced methods to determine the problem. These can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatments for toe pain and injuries vary and may include shoe inserts, padding, taping, medicines, injections, and in some cases, surgery. If you believe that you have broken a toe, please see a podiatrist as soon as possible.
If you have any questions please feel free to contact our office located in Gilbert, PA . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
What Is a Diabetic Foot Ulcer?

A diabetic foot ulcer, a grave complication for individuals with diabetes, is a chronic open sore that develops on the feet, typically on the bottom or sides. It arises from a combination of factors intricately linked to the effects of diabetes on the body. Diabetes can lead to neuropathy, causing reduced sensation in the feet and making it challenging to detect injuries or pressure points. Additionally, compromised blood circulation hampers the healing process, increasing the risk of infections and the formation of ulcers. Contributing further, the elevated blood sugar levels associated with diabetes impair the immune system, increasing the risk of infections. Foot ulcers, if left untreated, can escalate into serious complications and be quite painful. Recognizing the effects of diabetic foot ulcers underscores the importance of meticulous foot care in diabetes management. If you have diabetes and have developed a foot ulcer, it is suggested that you are under the care of a podiatrist who can effectively treat this type of wound, and help you to manage this condition.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Dr. Barbara Davis from Gilbert Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our office located in Gilbert, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
More...
Diabetic Foot Blisters

Diabetic foot blisters are a rare, but distinctive complication of diabetes. They typically manifest as painless blisters on the feet of people with diabetes, often without an obvious cause like injury or friction. These blisters can resemble burn blisters, presenting a risk for infection, especially given the compromised wound-healing abilities associated with diabetes. The skin of diabetic patients is vulnerable due to a combination of poor circulation, diabetic neuropathy, and other skin complications like dryness and poor healing. Management of diabetic foot blisters involves careful monitoring to prevent infection, control of blood sugar levels to aid in healing, and protection from further injury. In most cases, they may resolve on their own with good diabetes management and proper foot care, which includes wearing well-fitting shoes and avoiding walking barefoot. However, if you are diabetic and have any new or worsening foot issues, it is strongly suggested that you make an appointment with a podiatrist to ensure timely and appropriate treatment.
Blisters are prone to making everyday activities extremely uncomfortable. If your feet are hurting, contact Dr. Barbara Davis of Gilbert Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters develop as a result of constantly wearing tight or ill-fitting footwear. This happens due to the constant rubbing from the shoe, which can often lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
How Do Blisters Form?
Blisters on the feet are often the result of constant friction of skin and material, usually by shoe rubbing. Walking in sandals, boots, or shoes that don’t fit properly for long periods of time can result in a blister. Having consistent foot moisture and humidity can easily lead to blister formation.
Prevention & Treatment
It is important to properly care for the affected area in order to prevent infection and ease the pain. Do not lance the blister and use a Band-Aid to provide pain relief. Also, be sure to keep your feet dry and wear proper fitting shoes. If you see blood or pus in a blister, seek assistance from a podiatrist.
If you have any questions, please feel free to contact our office located in Gilbert, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
A Comprehensive Overview of Heel Spurs

Heel spurs, a common foot condition, are bony outgrowths that form on the underside of the heel bone. They often develop in response to long-term strain on the foot's ligaments and muscles. While many individuals have heel spurs, not all experience pain. When pain does occur, it is generally due to the inflammation of the surrounding tissues, a condition known as plantar fasciitis. The symptoms of heel spurs can include sharp, stabbing pain in the heel, especially while walking or standing after periods of rest. The pain tends to improve as the foot warms up but may return after prolonged activity. Risk factors for heel spurs include obesity, wearing poor-fitting or worn-out shoes, and activities that place excessive strain on the feet, such as running and prolonged standing. Diagnosis and treatment may involve having X-rays taken to confirm the presence of a heel spur. Understanding heel spurs and their management options is vital for individuals seeking relief from this often painful condition. If you have developed a heel spur, it is suggested that you consult a podiatrist who can determine if it is mild or severe, and offer treatment options that are right for you.
Heel spurs can be incredibly painful and sometimes may make you unable to participate in physical activities. To get medical care for your heel spurs, contact Dr. Barbara Davis from Gilbert Podiatry. Our doctor will do everything possible to treat your condition.
Heels Spurs
Heel spurs are formed by calcium deposits on the back of the foot where the heel is. This can also be caused by small fragments of bone breaking off one section of the foot, attaching onto the back of the foot. Heel spurs can also be bone growth on the back of the foot and may grow in the direction of the arch of the foot.
Older individuals usually suffer from heel spurs and pain sometimes intensifies with age. One of the main condition's spurs are related to is plantar fasciitis.
Pain
The pain associated with spurs is often because of weight placed on the feet. When someone is walking, their entire weight is concentrated on the feet. Bone spurs then have the tendency to affect other bones and tissues around the foot. As the pain continues, the feet will become tender and sensitive over time.
Treatments
There are many ways to treat heel spurs. If one is suffering from heel spurs in conjunction with pain, there are several methods for healing. Medication, surgery, and herbal care are some options.
If you have any questions feel free to contact our office located in Gilbert, PA . We offer the latest in diagnostic and treatment technology to meet your needs.
Children’s Foot and Ankle Injuries

Children often experience foot and ankle injuries due to sports, games, or falls. These injuries can range in severity, requiring different levels of medical attention. Ankle sprains happen when ligaments in the ankle stretch or tear due to rapid movements, often occurring during sports or high-energy activities. This can lead to swelling, pain, and bruising. Ankle strains involve muscle overstretching or tearing, which can be acute or chronic. Severe strains need immediate medical attention. Sever's disease causes heel pain in growing children, worsening with high-impact activities. It generally resolves over time. Ankle fractures are common in sports, and may involve any ankle bone. Complex fractures may necessitate surgery. Other injuries like puncture wounds, compartment syndrome, and ankle dislocations can occur and should be promptly treated by a podiatrist. If your child has a foot or ankle injury, it is suggested that you schedule an appointment with a podiatrist for a diagnosis and proper treatment.
The health of a child’s feet is vital to their overall well-being. If you have any questions regarding foot health, contact Dr. Barbara Davis of Gilbert Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Tips for Keeping Children's Feet Healthy
- Make sure their shoes fit properly
- Look for any signs of in-toeing or out-toeing
- Check to see if they have Clubfoot (condition that affects your child’s foot and ankle, twisting the heel and toes inward) which is one of the most common nonmajor birth defects.
- Lightly cover your baby’s feet (Tight covers may keep your baby from moving their feet freely, and could prevent normal development)
- Allow your toddler to go shoeless (Shoes can be restricting for a young child’s foot)
- Cut toenails straight across to avoid ingrown toenails
- Keep your child’s foot clean and dry
- Cover cuts and scrapes. Wash any scratches with soap and water and cover them with a bandage until they’ve healed.
If you have any questions, please feel free to contact our office located in Gilbert, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Risk Factors for Peripheral Artery Disease

Peripheral arterial disease, or PAD, is a vascular condition characterized by narrowed arteries in the legs, limiting blood flow to the feet. Several risk factors contribute to the development and progression of PAD. Smoking is a primary risk factor, as it damages blood vessels and promotes plaque buildup. Diabetes is another significant factor, as high blood sugar levels can damage arteries. Hypertension, or high blood pressure, places constant stress on arteries and can lead to their narrowing over time. Age is also a non-modifiable risk factor, as PAD becomes more common with advancing age. Genetics can play a role, with a family history of vascular diseases increasing one's susceptibility. Obesity and a sedentary lifestyle contribute by promoting the accumulation of fatty deposits in arteries. Additionally, high cholesterol levels can lead to plaque formation in blood vessels. Lastly, individuals with a history of heart disease are at higher risk for PAD. If you have risk factors for PAD or suffer from its effects on your feet, it is suggested that you schedule an appointment with a podiatrist for an examination and necessary treatment.
Peripheral artery disease can pose a serious risk to your health. It can increase the risk of stroke and heart attack. If you have symptoms of peripheral artery disease, consult with Dr. Barbara Davis from Gilbert Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Peripheral artery disease (PAD) is when arteries are constricted due to plaque (fatty deposits) build-up. This results in less blood flow to the legs and other extremities. The main cause of PAD is atherosclerosis, in which plaque builds up in the arteries.
Symptoms
Symptoms of PAD include:
- Claudication (leg pain from walking)
- Numbness in legs
- Decrease in growth of leg hair and toenails
- Paleness of the skin
- Erectile dysfunction
- Sores and wounds on legs and feet that won’t heal
- Coldness in one leg
It is important to note that a majority of individuals never show any symptoms of PAD.
Diagnosis
While PAD occurs in the legs and arteries, Podiatrists can diagnose PAD. Podiatrists utilize a test called an ankle-brachial index (ABI). An ABI test compares blood pressure in your arm to you ankle to see if any abnormality occurs. Ultrasound and imaging devices may also be used.
Treatment
Fortunately, lifestyle changes such as maintaining a healthy diet, exercising, managing cholesterol and blood sugar levels, and quitting smoking, can all treat PAD. Medications that prevent clots from occurring can be prescribed. Finally, in some cases, surgery may be recommended.
If you have any questions, please feel free to contact our office located in Gilbert, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.


